Pathophysiology
Current thoughts on the causes of narcolepsy:
A combination of these causes leads to dysfunctional synaptic transmissions, mainly in the pontine reticular activating system, which is a set of connected nuclei in the brain that is responsible for the sleep/wake cycle.
Very rare cases of narcolepsy are known to result from traumatic brain injuries and tumor growth in the regions of the brain that control REM sleep.
- Genetic predisposition: there are changes in several genes that influence the risk of developing narcolepsy. Even though most cases are sporadic, those with first-degree relatives that have been diagnosed with narcolepsy have a 40 times greater risk of developing the disorder.
- Abnormal neurotransmitter function: most people with narcolepsy have extremely low levels of the neurotransmitter hypocretin, also known as orexin, which promotes wakefulness.
- Abnormal immune modulation: when cataplexy is present, there is a discrete loss of brain cells that produce hypocretin. This is thought to be autoimmune in nature, and related to the human leukocyte antigen (HLA) complex.
A combination of these causes leads to dysfunctional synaptic transmissions, mainly in the pontine reticular activating system, which is a set of connected nuclei in the brain that is responsible for the sleep/wake cycle.
Very rare cases of narcolepsy are known to result from traumatic brain injuries and tumor growth in the regions of the brain that control REM sleep.
REM Sleep
|
Those with narcolepsy tend to exhibit dysfunction and inappropriate regulation of rapid eye-movement (REM) sleep. In a normal sleep cycle, people begin with non-REM sleep and transition to REM sleep within 80 to 100 minutes. Narcoleptics tend to enter REM sleep within a few minutes of falling asleep. REM sleep is controlled mainly by the pontine reticular activating system. In the brain, there are REM-on cells which fire only during REM sleep and REM-off cells which do the opposite. In narcolepsy, the inhibition of REM-on cells may be defective.
Symptoms present in narcolepsy can be characterized as REM sleep components intruding into wakeful states. For example, loss of muscle tone during cataplexy mirrors the interruption of muscle activity that naturally occurs during REM sleep. Hallucinations signify an intrusion of dreams, which also naturally occur during REM sleep. Scientists have learned that the group of neurons that becomes inactive during REM sleep also becomes inactive during cataplectic attacks, but further research needs to be performed in order to utilize this information. |
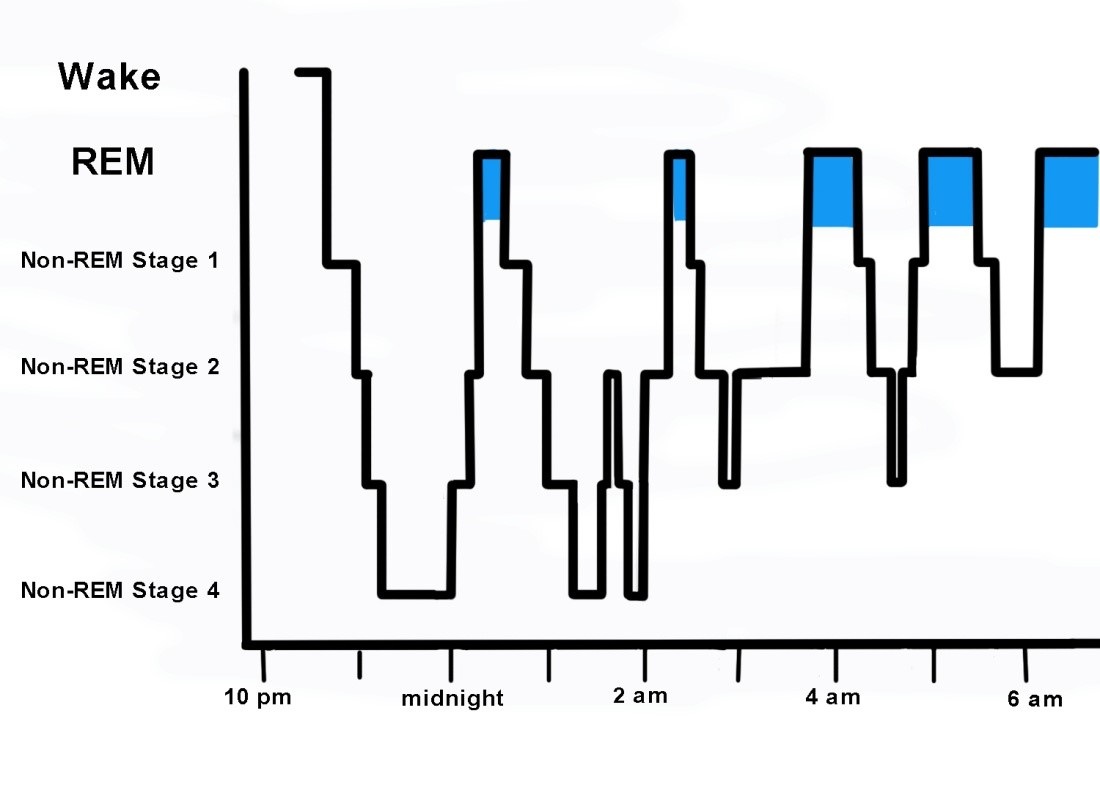
Graph of a normal sleep cycle. The blue highlights places where the individual was in REM sleep.
|
Signs AND Symptoms |
Narcolepsy & Cataplexy In Action |
|
The four most common symptoms of narcolepsy include:
|
|
- Cataplexy: This is the sudden loss of muscle tone while awake, which leads to loss of voluntary muscle control. Cataplexic attacks can occur during any time and vary greatly in severity. They can be as small as a mild drooping of the eyelid to as severe as a physical collapse in which individuals are unable to move, speak, or open their eyelids. Cataplexy is most common triggered by a strong and sudden emotion, such as fear, anger, stress, or excitement. The highest reported trigger of cataplexy is laughter. About 70% of people with narcolepsy also have cataplexy.
- Sleep Paralysis: This is the temporary inability to move while falling asleep or waking up. Attacks generally only last a few seconds or minutes, and people rapidly recover their full capacity to move and speak after it is over.
- Hypnagogic Hallucinations: This type of hallucination is related to sleep paralysis and occurs during sleep onset. The images are extremely vivid, seem life-like, and can be frightening. Hallucinations are primarily visual, but can involve any other sense as well.
"Narcolepsy ." Narcolepsy. N.p., n.d. Web. 01 Dec. 2014.
"What Narcolepsy Looks Like, Woman Films..." YouTube. YouTube, n.d. Web. 01 Dec. 2014.
"What Narcolepsy Looks Like, Woman Films..." YouTube. YouTube, n.d. Web. 01 Dec. 2014.